 Increasingly there is an expectation – quite rightly – that participation in clinical research should be an integral part of our practice as consultant breast surgeons. Clinical research allows us to create the evidence base we need to inform our clinical practice, while giving our patients the opportunity to participate in clinical trials of new treatments or technologies. Given that surgeons often act as leaders within their clinical teams, there are many opportunities for surgeons to contribute to research, and these are perhaps best summarised in Figure 1.
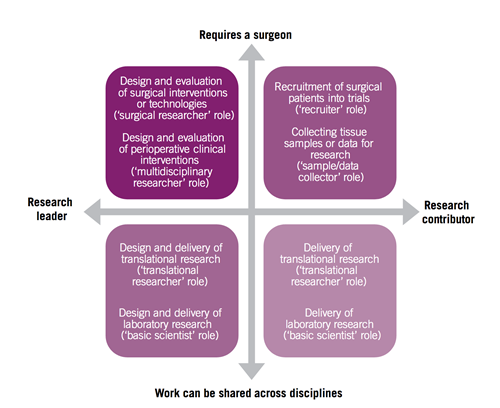
Increasingly there is an expectation – quite rightly – that participation in clinical research should be an integral part of our practice as consultant breast surgeons. Clinical research allows us to create the evidence base we need to inform our clinical practice, while giving our patients the opportunity to participate in clinical trials of new treatments or technologies. Given that surgeons often act as leaders within their clinical teams, there are many opportunities for surgeons to contribute to research, and these are perhaps best summarised in Figure 1.
Figure 1: From NCRI, Challenges and opportunities in surgical cancer research in the UK. October 2012
Getting involved in clinical research may be a daunting prospect, particularly for those with little or no previous experience in this area. For many, particularly newly appointed consultants, a first step may be to open or develop a portfolio of clinical trials within their unit (the ‘recruiter’ role in Figure 1). In this context, it’s important to recognise that clinical research is a team game, and it’s crucial to make sure that you have the support of your colleagues within the MDT. Many trials are multidisciplinary, and rely on the expertise of a variety of team members for successful delivery – the radiologists for collection of biological samples (such as tumour core biopsies) or the oncologists, for delivery of some systemic therapies in neoadjuvant or peri-operative studies. Experience suggests that it’s always better to get everyone on board before you start. It may also be more productive to try and open one or two trials in areas of real interest locally, where you feel that you will be able to recruit productively, than to try and open multiple trials and have limited recruitment, which can be frustrating and demoralising for everyone.
When it comes to negotiating your local hospital’s research governance procedures, or finding clinical research nurse (CRN) support “on the ground”, support is available through the National Institute of Health Research (NIHR) Clinical Research Network. The NIHR supports the setup and delivery of clinical research within the NHS through a network of Local Clinical Research Networks. Making contact with your LCRN will allow you to access the expertise and support necessary to deliver a trial within your unit. Most of the multicentre trials in breast surgery, such as POSNOC and LORIS, have been adopted onto the National Institute of Health Research (NIHR) Trials Portfolio and thus are eligible for support through the LRCNs. In my experience, a good working relationship and clear communication with your CRNs is essential to successful trial recruitment!
Some individuals may wish to extend their level of academic or research activity into some of the other roles outlined above, or indeed may be newly appointed academic consultants facing the challenges of reconciling the demands of a consultant post and a university appointment. Although tricky, there are a few things that I have found helpful over the last couple of years since taking up an academic post.
Having a job plan which allows the integration of these two aspects of an academic post is key to this. Having sufficient “chunks” of time to allow uninterrupted writing or data analysis is essential – and it’s important where possible to arrange a job plan that will accommodate this. However, I have found that maintaining some degree of separation of clinical and academic activity is necessary for academic productivity, while allowing me to concentrate on clinical issues on the days that I’m in the hospital. Having said that, a level of flexibility is sometimes necessary to facilitate the travel that’s often required in an academic post – whether to conferences, investigator meetings or other commitments away from home. This in turn means that it’s necessary to pay fairly close attention to both the diary of clinical commitments such as out-patient clinics and operating lists – as well as the on-call rota – to make sure that everything is covered (it sounds obvious but can rapidly become complex and challenging!).
Being able to manage deadlines (whether they are grant application deadlines, conference submission deadlines, or 31 day targets) can also prove daunting – I have found that keeping a well-ordered “to-do” list with deadline dates has been very helpful for my sanity. Linked to those deadlines are what seem like the interminable waits for feedback – so patience is vital; the research world proceeds at a different pace to the operating theatre. A thick skin is also a necessary attribute, as inevitably there are rejections and disappointments along the way. Having an experienced, senior mentor whose advice and input you trust can be invaluable, both in these situations, and in providing more general guidance as you develop your academic career. They may also be able to help you retain a focus on your key areas of interest and help you to recognise things that may detract from your key targets – learning to say “no” is never easy but it’s an essential skill, especially when you’re starting out. Maintaining a focus on “your” area of research can be difficult in view of all the competing and conflicting demands on your time, but it is vital.
With all this said, there is no doubt that incorporating academic and research activity in a consultant career – although challenging – can prove extremely satisfying. For me, some of the rewards include the continued intellectual stimulation of gaining new knowledge and skills, as well as the opportunities for multidisciplinary interaction that arise from research activity. Also, the blend of clinical activity, research (both clinical and translational) and educational activity that comes from an academic role allow a greater variety to the job than might be the case with a full-time NHS clinical consultant post.
Finally, although there may be challenges and obstacles, the most important qualities for success in integrating academic and research activity into a consultant career are probably enthusiasm and determination, with which almost anything should be possible!
Written by Stuart McIntosh,
Consultant Breast Surgeon, Queen's, University Belfast
